2 Studies Showing Doctors Still Rely on "Non-Evidence Based" Judgement in the Absence of RCT's
It's only certain covid treatments where there's nihilistic clinical paralysis
One of the more damning behaviors by the medical community throughout the pandemic was what Dr. McCullough termed “therapeutic nihilism” - the systematic refusal to even try treating covid patients. Doctors the world over fell victim to their own unique mass formation psychosis whereby they suddenly ‘forgot’ how to apply their knowledge and experience to a patient with a novel disease condition - in other words, the very act of “doctoring”.
The medical profession on an individual level seemed to initially adopt this new medical ethos more from fear of contracting covid themselves than anything else. However, in short order a philosophical theory to justify this mindset of doctoring obsoletion was constructed, a theory that was truly novel and a radical departure from canonical medical ethics going back millennia:
Any proposed treatment for covid by default was presumed to have an unfavorable risk/benefit profile compared with doing nothing & regardless of the risk covid itself posed to the patient with such a degree of certainty that it could only be dislodged by the most powerful form of evidence irrefutably proving otherwise.
(The motivations and/or deliberate intent by various people who promoted this behavior is its own complex subject that is beyond the scope of this article to address.)
This was all the more bizarre in light of the concurrent non-pharmaceutical interventions (NPI) that were broadly implemented in order to reduce transmission without any evidence for efficacy and without considering the calamitous toll such policies would inflict.
Two studies I recently came across highlight that the standard from before covid - try to treat using your best clinical judgement and expertise - is still standard for doctors, as long as it’s not the blacklisted cornucopia of covid pharma-/nutra-ceuticals, both of which are worth highlighting.
Study #1: Venous Thrombosis during Spaceflight
https://www.nejm.org/doi/full/10.1056/NEJMc1905875
This is a fascinating story in its own right. A group of astronauts doing a stint in the International Space Station were conducting ultrasounds on themselves to measure certain characteristics of blood in a zero-gravity environment. Lo and behold, they found a blood clot in the jugular vein one of the astronauts (definitely not a place you want to have a clot hanging out). The clot was only discovered because they were doing the ultrasounds, but had not caused any symptoms (“asymptomatic” clot), which was fortuitous because had it been left undiscovered, it could have eventually caused a serious medical event in space that might even have been fatal.
This presented a big conundrum to NASA. Blood clots in space are pretty uncharted territory for medicine. Definitely no big, fancy RCT’s to use. So did NASA just throw up their arms and say “wait until you have a stroke, and then it’s tough luck anyway because there are no operating theaters in space”? Nope. They.. wait for it… tried to figure out the pathology and come up with an ad hoc solution on the fly (pun intended) using the available information and resources at their disposal. *gasp*
First, they confirmed the diagnosis:
Follow-up ultrasound examination performed by the astronaut, guided in real-time and interpreted by two radiologists on Earth, confirmed the presence of venous thrombosis with subacute characteristics
With the diagnosis confirmed, NASA brought in a team of specialists to flesh out the many unknowns, and what medical interventions were available given the unique circumstances:
Multispecialty discussions ensued, weighing the unknown risks of thrombus embolism and retrograde extension into the sinus and cerebral veins against those of anticoagulation.
Using anticoagulants in space is not exactly a highly-developed sub-discipline of hematology, quite a bit could go wrong, and they had limited medical supplies - there’s no WalMart pharmacy up there:
Twenty vials containing 300 mg of enoxaparin each were available in the pharmacy of the space station, but no anticoagulation-reversal agent was available.
Long story short, what they did worked:
On landing, a point-of-care ultrasound examination revealed spontaneous flow in the supine position with residual thrombus flattened to the vessel walls (Fig. S1F), a finding consistent with images taken on the space station during the Müller maneuver; further anticoagulation was deemed unnecessary. Follow-up examinations revealed a small volume of residual thrombus 24 hours after landing and no thrombus 10 days after landing. A subsequent thrombophilia workup was unremarkable. On follow-up 6 months after the return to Earth, the astronaut continued to be asymptomatic.
The clincher is the following assessment by the authors of the study:
This case of venous thromboembolism in spaceflight highlights unique complexities of space medicine, such as the need for non–evidence-based clinical decision making; the need for patient-performed, radiologist-guided telemedicine ultrasonography; and a limited pharmacy in which long-term anticoagulation is not supported, syringes are a limited commodity, and drawing liquids from vials is a significant challenge because of surface-tension effects. Medical decisions in this case were implemented through concerted efforts across multiple space agencies to overcome the numerous logistic and operational challenges.
“such as the need for non–evidence-based clinical decision making”
“non–evidence-based”
😱😱😱😱😱😱😱😱😱
We could be forgiven for thinking that this is the highest of high medical heresies. Making treatment decisions that are NOT EVIDENCE BASED?????
Snarkiness aside, what we see here is the intuitive application of the best expert judgement applied to a novel clinical situation where they didn’t have an official protocol to go by. Rather, as articulated by the rest of this paragraph, the expert clinical team assembled by NASA did the best they could with what they had. In other words, they followed standard medical practice and ethics to treat patients as best they were able in the circumstances they found themselves in.
One final observation is in order. Considering that NASA had about 90% of their workforce vaccinated by November 2021, let’s just say that they should indeed anticipate lots of good ole’ clotting:
In addition, the observed blood-flow anomalies reveal gaps in our understanding of circulatory and hemostatic physiology.4 Although cervicocranial venous overcapacity is a known effect of spaceflight, the resultant changes in flow organization, local whole-blood viscosity, and prothrombotic risk need exploration. Active astronaut surveillance and experimental models are critical to the development of prevention and management strategies for venous thromboembolism in weightlessness, especially with future plans for prolonged space travel to the Moon and Mars.
We should probably expect to see ‘accelerated’ development to the field of spaceflight hematology.
Study #2*: Case Report of Vaccine Injury, Treatment and Subsequent Vaccination with Dose 2
*This is really a category of studies as there are multiple case reports where a patient was given dose 2 despite a SAE following dose 11.
Third cranial nerve palsy in an 88-year-old man after SARS-CoV-2 mRNA vaccination: change of injection site and type of vaccine resulted in an uneventful second dose with humoral immune response
https://pubmed.ncbi.nlm.nih.gov/35135792/
We’ll let the authors tell the story of this 88-yo victim of vaccine injury:
Three days after the first administration of Moderna mRNA-1273 SARS-CoV-2 vaccine in the right deltoid, he was brought to the emergency department for objective dizziness, diplopia and gait instability.
The patient (weight 65 kg) received prednisone 25 mg/day (0.38 mg/kg/day) for 1 week then gradually tapered off over a period of 2 weeks until suspension. This steroid schedule was at a lower dose than that usually adopted for the treatment of cranial nerve palsies,4 but eventually led to a fast recovery of the clinical manifestations in our patient after 5 days of treatment.
Here’s where things get interesting. To treat the palsy, they used corticosteroids. There’s a significant drawback to the use of steroids in the context of vaccines: because they suppress the immune system, the immune system won’t react to the vaccine itself either that had just been given to this patient. With this in mind, the treating physicians decided to use a lower dose of steroids than was typical in this context in the hopes that they could salvage some vaccine efficacy in the sense of developing antibodies and other covid-specific immune cells:
The choice to adopt a lower dose of steroids was undertaken in consideration of the age of the patient and in order to try not to blunt the vaccine response.
They were partially successful, although the patient did not develop detectable antibodies to covid, they were able to find some covid-specific T-Cells:
However, serum antibodies against the SARS-CoV-2 receptor-binding domain (RBD), performed by luciferase immunoprecipitation system (0.24 arbitrary units (AU)) and by routine assay (<0.4 U/mL),5 6 resulted negative 2 and 3 weeks after vaccination, respectively. On the other hand, T cell proliferative responses to the SARS-CoV-2 S protein were detectable (Stimulation Index (SI): 19), along with normal proliferative responses to mitogens (PHA, anti-CD3) as well as to other viral antigens (Cytomegalovirus, Varicella-Zoster virus, Herpes simplex virus).
The authors concluded that the steroids were responsible for the failure of the vaccine to elicit any antibodies:
This suggested that, in the presence of a normal T cell response, the steroid course may have had mainly blunted the humoral responses.
At this point, the doctors were facing a dicey situation. On the one hand, their patient - a fragile 88yo man with a whole laundry list of comorbidities - had not developed functional immunity to covid, and so was at severe risk from covid.
On the other hand, the first dose of the vaccine had provoked a severe neurological deficit. Even though they had been able to treat it successfully, there was no guarantee that a second recurrence following a second vaccine dose would be just as treatable as the first go around.
Critically, there was no available data, let alone a full-blown RCT, on the risks of an SAE following dose 2 after a dose 1 SAE, regardless of which vaccine or combination of vaccines were used.
With that context, let’s return to the case report. They decided to go ahead with dose 2, but with Pfizer instead of Moderna:
Given the fragility of the subject and his high-level risk of COVID-19, the treating physician considered a positive benefit–risk ratio in favour of a full immunisation with a second dose of a different vaccine to decrease the risk of an AE recurrence.
Empirically, a dose of Pfizer mRNA-BNT162b2 SARS-CoV-2 vaccine in the left quadriceps femoris, contralateral to the first vaccine site and nerve paralysis, was administered, in order to reduce the risk of proximity to a potential inflammatory/immune reaction.
Aaaand…..
Their gambit worked out:
In point of fact, the second vaccine administration was uneventful and resulted in a further increase of T lymphocyte proliferative response specific to the SARS-CoV-2 S peptide (SI: 45). Of note, a robust IgG titre to RBD (272.8 AU) and spike proteins (S2 474.3 AU) was also detected 3 weeks after.
The patient was followed up with serial clinical evaluations and did not show any signs or symptoms after the second vaccine administration.
To reiterate, yes, in this case their (gutsy) wager succeeded2.
Let’s recap:
The doctors faced a novel clinical situation - a patient at profound risk from covid but who suffered a SAE from vaccine Dose #1. They had no RCT’s (or any evidence frankly) to guide their decisions. So they made do and used ‘non-evidence based’ judgement… to prophylactically treat a patient to prevent him contracting covid3.
Takeaway: Doctors are perfectly happy to use “non-evidence based judgement”
Both studies show that in the absence formal protocols or guidance to turn to, doctors make do without them and forge ahead regardless. Unlike their attitude regarding covid infection, they didn’t throw their hands up and say “oh well”.
The case report study is particularly instructive, because it pertained to covid. The doctors in this instance decided to vaccinate the patient with dose 2 despite having no data on safety or efficacy. They did not know whether dose 2 would result in another bout of Bell’s palsy, or an even worse neurological or other condition/s. They also could not predict efficacy, and there was the distinct possibility that they would have to treat the patient with more steroids in response to a dose 2 SAE that would blunt or altogether neutralize the vaccine itself.
Compare this to treating covid itself (before the public awareness that monoclonal antibodies for covid existed or the advent of Paxlovid or Mulnopiravir): This same patient would have been told to go home and do nothing despite the “fragility of the subject and his high-level risk of COVID-19” would he have contracted covid in 2020.
‘It’s the incentives, stupid’
People generally act in consonance with what they are incentivized to do.
The difference between the routine situations where “non-evidence based decision making” is a reflexive “duh of course” versus covid treatment - especially the backlisted treatments - is really just a question of incentives.
In the first study, NASA was heavily incentivized to make every possible effort to save their astronaut. An astronaut dying in space is a big deal, and also a very expensive big deal. Furthermore, if NASA would abandon their astronaut to medical calamity, NASA’s ranks would be quickly depleted of astronauts, who would be understandably recalcitrant to put their lives in the hands of an agency who had just demonstrated blatant disregard for their welfare and lives.
In the second study, the doctors had a slew of incentives, including interest in the patient’s welfare, “vaccine virtuousness”, the novelty of being on the cutting edge of medical discovery4, and an institutionalized medical community culture heavily in favor of indiscriminate mass vaccination.
Similarly for the NPI’s implemented to reduce covid transmission, various groups of people were heavily incentivized to implement or consent to the aggressive and draconian policies enacted. Panicky doctors (and laypeople) facing what they perceived to be an apocalyptic terror were not about to get hung up on the trivialities of evidentiary standards. Politicians and others who stood to benefit from ‘not letting a crisis go to waste’ likewise pounced on the opportunity to achieve [evil] policy goals previously thought to be out of reach or impossible.
When it came to treating covid however, your average doctor was heavily disincentivized from treating covid especially using the “blacklisted” drugs by a vast array of incentives ranging from FDA warnings of toxicity to their own cognitive dissonance that they would feel for failing to have treated covid patients were covid indeed easily treatable to threats against their careers and social lives5. And some highly placed individuals within the institutional hierarchy of medicine had insidious motivations such as preserving the market for expensive novel Pharma products or inflicting various transformations upon the political structures and institutions of the world.
There’s a critical exception to this that proves the rule: Dr. Kory reported6 that after the first few months of covid, nursing homes tried Ivermectin and saw that it worked, which was a big part of why nursing homes were a tiny % of covid deaths after being responsible for the lion's share of covid mortality at the beginning.
What made nursing homes different was that unlike hospitals, nursing homes and other types of long-term care facilities only make money on patients who are living. Thus they were incentivized to keep their patient populations alive, which they did. (It helped that nursing homes have in-house pharmacies too, so they could compound their own Ivermectin without dealing with the government bureaucracies or medical cartel organizations.)
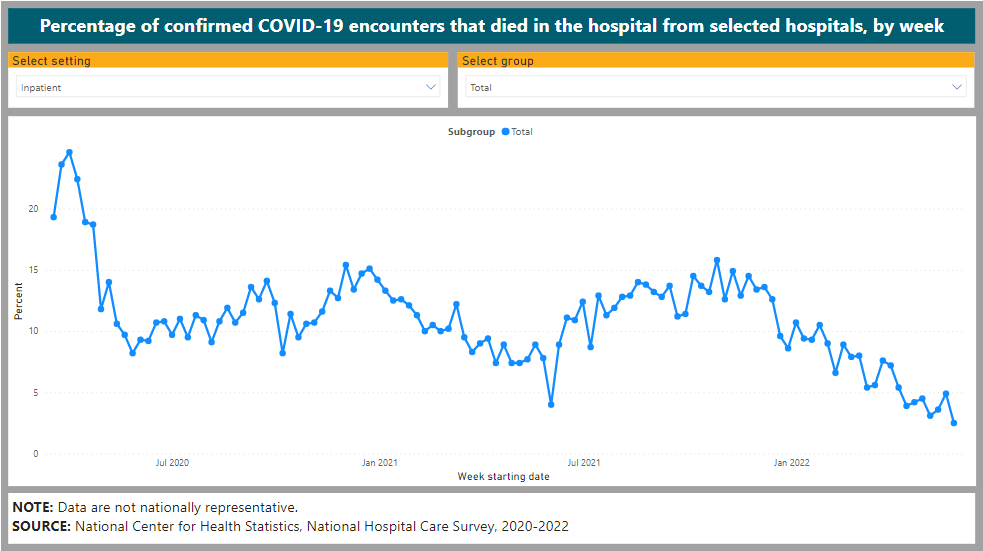
Compare nursing homes to hospitals who were financially incentivized to fraudulently inflate covid case numbers; to give all “covid” patients the highly toxic Remdesivir7; and to ventilate patients, among other perverse incentives rewarding hospitals for grotesquely abusing patients. Hospital mortality in the US remained elevated throughout the pandemic, only starting to come down once Omicron took over and pretty much everyone already had some degree of natural immunity (I have a graph somewhere from FLCCC analyst Juan Chamie showing the drop in % of covid deaths from nursing homes / LTC facilities that I can't find right now).
I am focusing here specifically on the mindset of the doctors regarding their decision making in the absence of evidence, not the other profoundly immoral aspects.
It’s important to be honest and accurate about the facts, and in this instance, the patient was vaccinated with Pfizer Dose 2 without a subsequent SAE. The positive outcome does not excuse making such a reckless and unjustified gamble in the first place, it would be akin to playing Russian Roulette and declaring after surviving that this proves that it was a good decision to play in the first place.
The doctors here clearly have a ridiculous myopic obsession with covid and generating antibodies to covid.
“The outcome of SARS-CoV-2 immunisation and the continuation of the immunisation programme in these subjects have not been explored to date in the scientific literature.”
Going through all the relevant incentives here would need its own article.
on FLCCC zoom & I’m pretty sure in at least one of his substacks but I don’t remember where either of them are
For the record, this means that hospitals were likely administering Remdesivir to some number of ‘asymptomatic incidental covid’ patients. This is probably part of the reason for the US’s absurdly high covid mortality compared to the rest of the world - if you give Remdesivir to trauma patients from car accidents who happen to test positive for covid, that’s probably going to lead to worse outcomes for trauma patients - that will then be labeled “covid deaths”.




I am deliberately choosing to tone down the criticism of the establishment. One of my goals on substack is to write pieces that can be shared with people who are not yet on our side. If they are written with the appropriate measure of condemnation of the "bad guys", they will come across to such individuals as highly inflammatory and uncredible.
Furthermore, my objective with this post is specifically to highlight how doctors when it comes to other things still follow the age old standard of "do something" and don't get nitpicky about the lack of available big, fat glorious RCT's.
I get the spirit of this. But as a former practicing MD, this was a case of:
1. Don’t just do something, stand there!
2. Because of Covid, doctors have shown that today, more than ever, they are owned by big pharma and the hospital system and given a choice between their livelihood and the lives of their patients, guess what they picked.